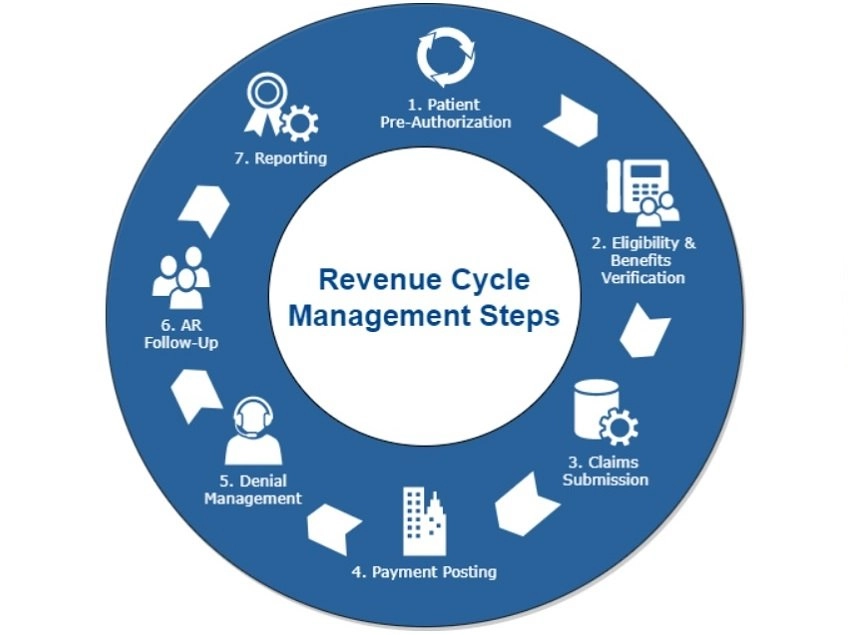
Revenue cycle management (RCM) is the financial process that healthcare facilities use to track patient care episodes from registration and appointment scheduling to the final payment of a balance.
All the administrative and clinical functions, processes, and software applications that contribute and manage the registration, charging, billing, payment and collections tasks associated with a patient encounter.
Revenue cycle is the process that begins when a patient comes into the system and includes all those activities that have occurred in order to have a zero balance.
Revenue cycle management unifies the business and clinical sides of healthcare by coupling administrative data such as a patient’s name, insurance provider and other personal information and the treatment a patient receives.
RCM Functions
Encounter
- Insurance Verification
- Registration scheduling for a clinic
- POS collections Cash handling
Collection
- Contractual Payment terms
- Contractual allowance
- Denial management
- Reconciliation
- Refunds
Contract Compliance
- Contract terms
- Policy Validation
- Approvals Referrals
Billing
- Claims Review
- Claim Edits
- Claim Submission
- Secondary Claims
- Reconciliation
Stay Management
- Effective documentation
- Stay reviews
- Denial Management
- Length of stay
- Discharge planning
- Denials/appeals
Charge Capture
- Charge entry
- Charge review
- Charge reconciliation
- Late charges
- Lost charges

Revenue Cycle Management Value Proposition:
- Increased average of claims paid after 1st submission
- Reduced denial rate
- Improved net revenue to the practice
- Higher percentage of clean claims
- Reduced outstanding accounts receivables
- Faster claims payment
- Less lost claims
- Improved quality of care by having more time for patient care issues
- Correct patient information available and less stress to your staff